
Shining a light on PIMS-TS
( Paediatric Multi-inflammatory Syndrome temporally associated with SARS-CoV-2 )
( Paediatric Multi-inflammatory Syndrome temporally associated with SARS-CoV-2 )
Family Stories
"Wisdom is the
reward of experience
and should be shared."
reward of experience
and should be shared."
Image: https://wallpaperaccess.com
The following family testimonies are shared with you so that you can have a better understanding of PIMS-TS. It is traumatic, but by knowing what to look for and what to expect, we hope you will be better prepared should this happen to your child and hopefully help you reach a prompt diagnosis. If your child shows the symptoms of PIMS-TS, please join our Facebook support group, where our families will be happy to support and guide you.
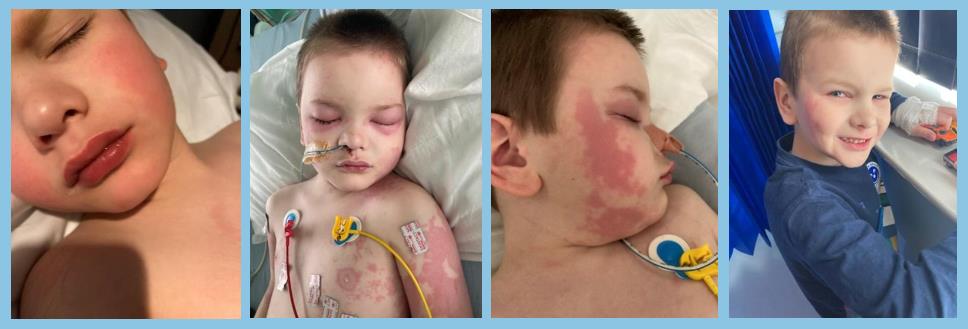
Oliver’s Story, age 6, told by his mum, Laura
In March 2021, Oliver, aged 6, tested positive for Covid. I wasn’t too concerned as he was asymptomatic. Three weeks later Oliver lost his appetite and developed a tummy ache. After another week he became lethargic, light sensitive and his stomach pain worsened. I took him to Urgent Care, where he was diagnosed with tonsillitis and sent away with antibiotics. Something didn’t feel right so I took him to A&E to get a second opinion. Again, he was diagnosed with tonsillitis and sent home, but on our way out of hospital he vomited. He was admitted, and over the next 24 hours Oliver developed a persistently high temperature, a blotchy rash on his arms and face, painful eyes, and red lips, palms, feet and eyelids. At this point the doctors started mentioning Kawasaki Disease and PIMS-TS. I had never heard of either.
In March 2021, Oliver, aged 6, tested positive for Covid. I wasn’t too concerned as he was asymptomatic. Three weeks later Oliver lost his appetite and developed a tummy ache. After another week he became lethargic, light sensitive and his stomach pain worsened. I took him to Urgent Care, where he was diagnosed with tonsillitis and sent away with antibiotics. Something didn’t feel right so I took him to A&E to get a second opinion. Again, he was diagnosed with tonsillitis and sent home, but on our way out of hospital he vomited. He was admitted, and over the next 24 hours Oliver developed a persistently high temperature, a blotchy rash on his arms and face, painful eyes, and red lips, palms, feet and eyelids. At this point the doctors started mentioning Kawasaki Disease and PIMS-TS. I had never heard of either.
By Day 3, the rash had spread across Oliver’s body and his temperature couldn’t be kept down with paracetamol. An ultrasound showed inflammation around his stomach and gall bladder. The doctors settled on Kawasaki Disease and started treatment of immunoglobulin. However, that night Oliver’s blood pressure dropped significantly and he was transferred by ambulance to the Evelina Paediatric Intensive Care Unit. By Day 4, the inflammation markers in Oliver’s blood reached 338 (they should be less than 10), the rash continued to spread, his temperature passed 40 and he developed swelling to his face. At this point the consultants called Oliver a ‘diagnostic conundrum’. They were considering Kawasaki disease, PIMS, sepsis and autoimmune diseases, but Oliver didn’t fit the criteria for one particular condition and the immunoglobulin hadn’t worked.
On Day 5, Oliver became very sick. His heart function deteriorated and the doctors struggled to stabilise him. He was finally diagnosed with PIMS-TS and was given IV steroids, antibiotics, and adrenaline, noradrenaline and milrinone to support his heart. Over the next 2 days the inflammation markers in his blood continued to rise and the doctors were concerned that Oliver hadn’t responded to the IVIG or steroids. He was given an additional course of steroids and a drug called Tocilizumab to effectively switch off his immune system. By Day 8, Oliver had turned a corner and left intensive care. After 2 weeks in hospital and many ultrasounds, ECG’s, echocardiograms, MRI scans and blood tests, we were discharged with steroids, aspirin and antibiotics to take at home. He had a heart scan at 2 weeks, 3 months and 8 months post discharge, and we are very lucky that he has recovered well and his heart has returned to normal.
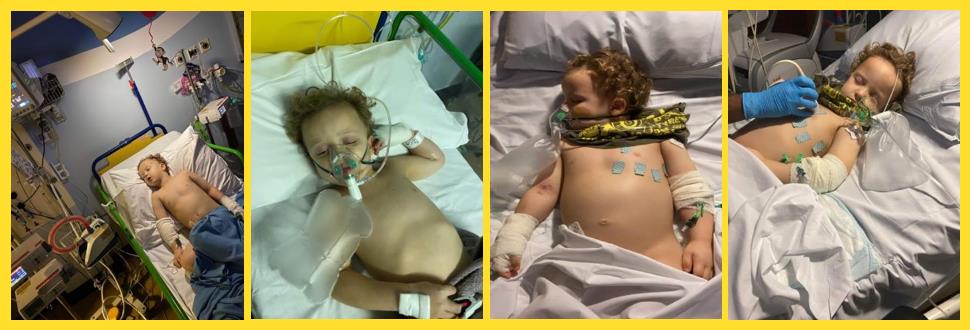
Rapha’s Story, age 3 told by his mum, Jo
On 12th September 2021 my 3-year-old son Rapha tested positive for COVID. He suffered for 2 days then recovered. A month later he started with a fever. After 24 hours it was getting worse. I took him to the GP who sent him home with the advice to give paracetamol and ibuprofen until he improved. Two days later he deteriorated and a paramedic came. He ended up in A&E, who dismissed him the moment the doctor saw him with “it’s viral”. For 3 more days he continued with the fever but now he was also constantly crying in pain, sometimes screaming, his head hurt, his eyes hurt, his tummy hurt. He became doubly incontinent, his eye whites turned pink, his lips cracked and his tongue swelled. I took him back to A&E who rushed him through immediately. After many investigations and MDT meetings with the nearest hospital that had a children’s ITU, we discovered that he had developed PIMS-TS. At this point Rapha was not lucid at all and required morphine for his pain and oxygen therapy. The surgical team reviewed him due to how swollen he was and he had a CT scan of his abdomen. His spleen was enlarged and he had fluid building up. His platelets were being destroyed, his literal insides were inflamed and he was in so much pain.
On 12th September 2021 my 3-year-old son Rapha tested positive for COVID. He suffered for 2 days then recovered. A month later he started with a fever. After 24 hours it was getting worse. I took him to the GP who sent him home with the advice to give paracetamol and ibuprofen until he improved. Two days later he deteriorated and a paramedic came. He ended up in A&E, who dismissed him the moment the doctor saw him with “it’s viral”. For 3 more days he continued with the fever but now he was also constantly crying in pain, sometimes screaming, his head hurt, his eyes hurt, his tummy hurt. He became doubly incontinent, his eye whites turned pink, his lips cracked and his tongue swelled. I took him back to A&E who rushed him through immediately. After many investigations and MDT meetings with the nearest hospital that had a children’s ITU, we discovered that he had developed PIMS-TS. At this point Rapha was not lucid at all and required morphine for his pain and oxygen therapy. The surgical team reviewed him due to how swollen he was and he had a CT scan of his abdomen. His spleen was enlarged and he had fluid building up. His platelets were being destroyed, his literal insides were inflamed and he was in so much pain.
He was put on fluids as he was not eating, morphine for the pain, antibiotics (as part of the sepsis protocol), and was put on immunoglobulin therapy. Unfortunately the immunoglobulin was not successful and Rapha was put on the second line treatment of methylprednisolone for 3 days. This treatment worked, and effectively stopped his immune system from attacking him. He had some further issues to contend with such as hypalbuminaemia which led to his whole body swelling up and he required an albumin infusion, as well as infusions of potassium and phosphate as those levels also dropped dangerously low. Echocardiograms of his heart showed an aneurysm had formed in his left coronary artery and he was placed on anti-platelet therapy to prevent that getting worse. Rapha’s mobility suffered and he required physiotherapy to build his muscles and strength up so that he could sit and walk again.
Rapha came home after a couple of weeks and has had regular follow up appointments, blood tests, ECG’s, echocardiograms, and physiotherapy. He is now back at swimming and rugby lessons and coping well with life. He often tells his consultant “no sharp things today” but the memories of painful catheterisations, cannulations and stomach decompressions are fading for him now. He remains on anti-platelet therapy and gastric protection. His cardiologists are certain that his heart will fully recover. I struggle when I think how many times I told him to calm down in the initial days of his fever. I believed the doctors who told me it was “just viral” when he was genuinely in pain and needing urgent treatment. The consultant said “it’s a good thing you brought him when you did” - a sentence that has scared me. I wish that Rapha’s story can help other parents advocate better for their children if they develop PIMS.
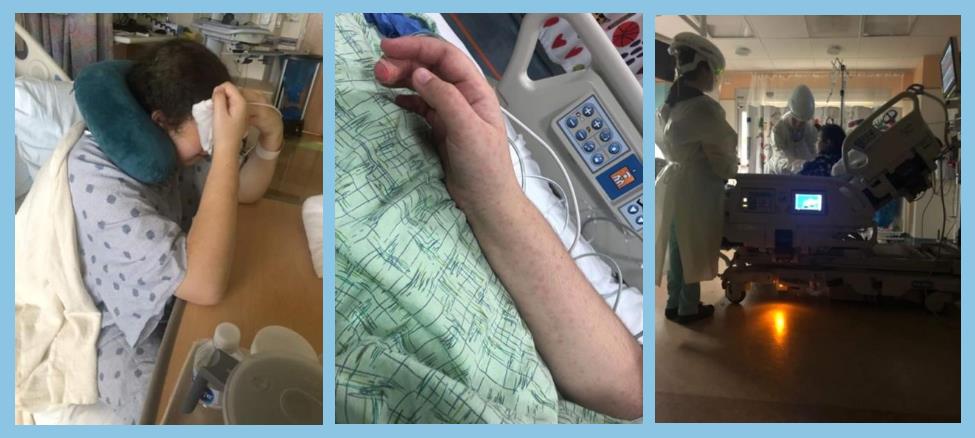
Kaylen’s Story, told by her mum, Melissa (Based in US)
One day in September 2021 I woke all 3 of our children up and we came downstairs to watch the livestream of our church. My middle daughter, Kaylen, complained of a headache, but with a teenager, that was nothing new. I gave her some ibuprofen and we finished up church. About an hour later she said her headache was worse and she had glassy bloodshot eyes (my clue that she had a fever). I checked and sure enough, 101.5. I told her to get in bed. About 30 min later she started complaining of chest pain and shortness of breath. This scared me enough to take a trip to the ER. At the ER they noticed her heart rate was in the 140s. After a VERY long day and oodles of tests, the paediatrician at the hospital said he thought our daughter would be more comfortable at home in her own bed and released us. (That was 10pm).
One day in September 2021 I woke all 3 of our children up and we came downstairs to watch the livestream of our church. My middle daughter, Kaylen, complained of a headache, but with a teenager, that was nothing new. I gave her some ibuprofen and we finished up church. About an hour later she said her headache was worse and she had glassy bloodshot eyes (my clue that she had a fever). I checked and sure enough, 101.5. I told her to get in bed. About 30 min later she started complaining of chest pain and shortness of breath. This scared me enough to take a trip to the ER. At the ER they noticed her heart rate was in the 140s. After a VERY long day and oodles of tests, the paediatrician at the hospital said he thought our daughter would be more comfortable at home in her own bed and released us. (That was 10pm).
We came home, but there was no way I could sleep. I checked on her at 11pm and her fever was 104 and her heart rate 169. Back to the ER we went. This time the paediatrician decided to transport us to Children's Hospital in DC. Another 18 hours in an ER room at Children's before they had a bed for Kaylen. They were ruling out all kinds of scary things (blood clot, meningitis, myocarditis etc), but this was the first time I heard of possible MIS-C (Multisystem Inflammatory Syndrome in Children).
After 30+ hours in different ERs and ambulances we were finally put in the nicest room in the hospital with the amazingly sweetest nurse. Too bad that only lasted a few hours before my daughter started crashing. Her blood pressure kept falling and our nurse called for a rapid response team... Pretty soon we had over 12 doctors in her room all scrambling to decide what to do. We were transferred to the ICU from there.
A couple of days in the ICU and they decided that she did indeed have MIS-C. She got some life-saving (IVIG) meds and some bad reactions to that (which also scared this mama... another rush of doctors to make sure my daughter didn't have a brain bleed, meningitis (caused by the meds) stroke or other brain complication).
But as quickly as it came, it left (not without some damage and oodles of follow ups with cardiology, haematology, rheumatology, infectious disease and her paediatrician).
But as quickly as it came, it left (not without some damage and oodles of follow ups with cardiology, haematology, rheumatology, infectious disease and her paediatrician).
I am not writing this to scare you - I just want to get the word out there. Act quickly if you see symptoms.
Kaylen was a bit unique since she was almost fully vaccinated against Covid, but this still came as a reaction to being exposed to Covid at some point.
Kaylen was a bit unique since she was almost fully vaccinated against Covid, but this still came as a reaction to being exposed to Covid at some point.
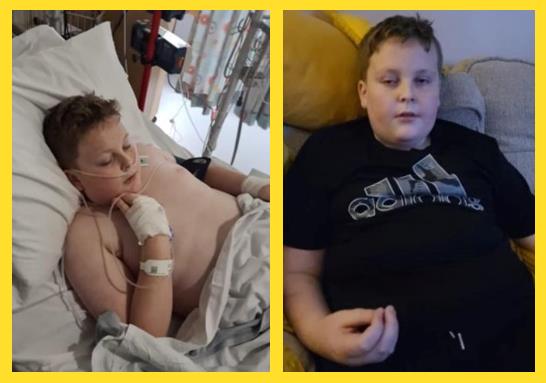
Jack's story, age 12, told by his mum, Allison
In November we all had covid but Jack wasn't ill and got through it without a problem.
On Boxing Day he complained of feeling sick and having stomach-ache. He then had what we thought was a stomach bug. Then on New Year’s Eve he became very ill. Eyes swollen, high temp, breathing very fast, fast pulse. After asking advice from a friend we called an ambulance. They came and assessed him and put him on oxygen as his levels were low. Blood pressure low and heart rate up. Took him to A&E where bloods were taken, cannula in etc. We were very lucky that the consultant on duty was one of the few involved in the PIMS study and he recognised it straight away. Jack was taken to HDU, more tests were done and the next day IVIG treatment was given.
In November we all had covid but Jack wasn't ill and got through it without a problem.
On Boxing Day he complained of feeling sick and having stomach-ache. He then had what we thought was a stomach bug. Then on New Year’s Eve he became very ill. Eyes swollen, high temp, breathing very fast, fast pulse. After asking advice from a friend we called an ambulance. They came and assessed him and put him on oxygen as his levels were low. Blood pressure low and heart rate up. Took him to A&E where bloods were taken, cannula in etc. We were very lucky that the consultant on duty was one of the few involved in the PIMS study and he recognised it straight away. Jack was taken to HDU, more tests were done and the next day IVIG treatment was given.
Jack was on oxygen, antibiotics, fluids, aspirin, injections in stomach and bed bound.
Within 24 hours he was sitting up and eating for the first time in days.
Heart scan was done and showed no damage but we will have follow ups to check.
Discharged on the 5th Jan and had a follow up 2 weeks later.
Still on iron, aspirin and calcium but getting stronger each day and went back to school for a couple of hours each day starting last week.
Within 24 hours he was sitting up and eating for the first time in days.
Heart scan was done and showed no damage but we will have follow ups to check.
Discharged on the 5th Jan and had a follow up 2 weeks later.
Still on iron, aspirin and calcium but getting stronger each day and went back to school for a couple of hours each day starting last week.
Cai’s story, age 9, told by his mum, Sally
Cai had covid 31 October but was pretty much asymptomatic. Fast forward 4 weeks later he started to complain of neck pain on the right side of his neck. As he plays football 6 times a week we put it down to muscular pain. A day later he seemed to run a high fever, so we were concerned about meningitis. We phoned our local GP who insisted we go to our local A&E; they don't provide a Paediatric service but told us to go there initially. We visited that morning and Cai was diagnosed with Wry neck (torticollis), his fever wasn't addressed. I came away not feeling convinced.
Cai had covid 31 October but was pretty much asymptomatic. Fast forward 4 weeks later he started to complain of neck pain on the right side of his neck. As he plays football 6 times a week we put it down to muscular pain. A day later he seemed to run a high fever, so we were concerned about meningitis. We phoned our local GP who insisted we go to our local A&E; they don't provide a Paediatric service but told us to go there initially. We visited that morning and Cai was diagnosed with Wry neck (torticollis), his fever wasn't addressed. I came away not feeling convinced.
That same night we drove to our closest Paediatric A&E in Carmarthen. Again, he was diagnosed with Wry neck and scarlet fever, as he was extremely flushed. The Friday he didn't seem to get any better. By Saturday afternoon Cai's face had dropped on one side, his neck was red and swelling and he was drooling a lot. We went back to Glangwilli Hospital, where initially they diagnosed him with an abscess in his neck. They gave him a CT scan that night, where it showed no sign of an abscess.
He was then assessed by the ENT doctor who diagnosed him with an infection of the lymph nodes. He was admitted to hospital and administered with antibiotics that night. The next morning, his PCR test that he had to take on admission came back positive. The nurses put us into an isolation room. I explained that he tested positive a month ago and thought that it could still be in his system. The doctors told me that it would be in his system for 60 days and this is what set alarm bells ringing. One of the doctors mentioned PIMS but his inflammatory markers at the time were borderline so they continued to treat for the infection. Cai wasn't getting any better so repeated his bloods on Tuesday. This time his inflammatory markers had increased to 248. This time, along with the Infectious Diseases Dept in Cardiff, he was diagnosed with PIMS.
We were immediately moved to a side room where he could be closely monitored. He was put on steroids straight away, along with his antibiotics and given numerous ECG's and x-rays.
We were immediately moved to a side room where he could be closely monitored. He was put on steroids straight away, along with his antibiotics and given numerous ECG's and x-rays.
The next day he had a cardiac echo which showed that his heart wasn't contracting properly and he had a leak in one of his valves. He remained on a heart monitor as his blood pressure was low and his pulse rate was also low. If it went below a certain point they would then have to treat him for heart failure. Thankfully it never came to that. After 4 days of being on steroids Cai improved so much that we were discharged. He received another echo two days after discharge, when there was an improvement on his heart. Our 8 week follow up appointment is on Wednesday, so we are keeping everything crossed for some good news, and that he can slowly start to return to football.
Maddie’s story, age 9, told by her mum, Jude
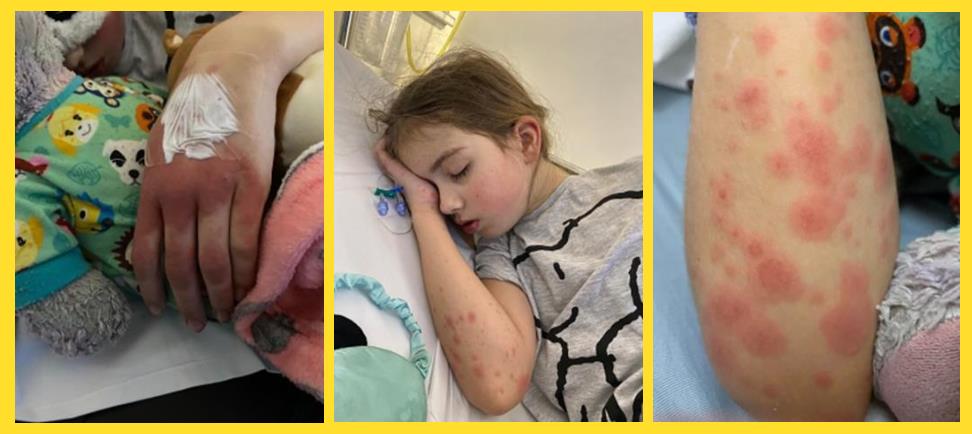
Sunday 16th January we took Maddie to urgent care with a rash that started on feet and hands with temperature of 39. Diagnosed with hand foot and mouth, when the nurse pressed Maddie tummy it was painful. The nurse spoke to a surgeon with concerns over appendicitis, but he/she wouldn’t see Maddie as the main symptom wasn’t tummy pain. We were advised to take Maddie back if she got worse and told hand foot and mouth plus high temperature would take a week to go. I had every intention of taking her back to be checked over again as I knew something was wrong. Later that evening Maddie’s temperature want up to 40, she’d been sick, so I took her straight back. This time we were sent to children’s ER. Within 20 minutes of getting there Maddie suddenly went from walking round to ER and being very alert and aware of her surroundings to not knowing who I was, very delirious, confused and crying out in pain. Admitted to HDU Children’s ward and started on IV antibiotics and paracetamol plus ibuprofen to treat her for meningitis and encephalitis, blood tests done and put on heart monitor. Overnight Maddie was sleeping or crying out in pain.
Sunday 16th January we took Maddie to urgent care with a rash that started on feet and hands with temperature of 39. Diagnosed with hand foot and mouth, when the nurse pressed Maddie tummy it was painful. The nurse spoke to a surgeon with concerns over appendicitis, but he/she wouldn’t see Maddie as the main symptom wasn’t tummy pain. We were advised to take Maddie back if she got worse and told hand foot and mouth plus high temperature would take a week to go. I had every intention of taking her back to be checked over again as I knew something was wrong. Later that evening Maddie’s temperature want up to 40, she’d been sick, so I took her straight back. This time we were sent to children’s ER. Within 20 minutes of getting there Maddie suddenly went from walking round to ER and being very alert and aware of her surroundings to not knowing who I was, very delirious, confused and crying out in pain. Admitted to HDU Children’s ward and started on IV antibiotics and paracetamol plus ibuprofen to treat her for meningitis and encephalitis, blood tests done and put on heart monitor. Overnight Maddie was sleeping or crying out in pain.
The following morning a doctor examined Maddie; the rash had got much worse and spread to her arms, legs, back, tummy and chest. She also had flushed face and bright red lips. As Maddie wouldn’t move her neck much they were going to do a lumbar puncture to test for meningitis and encephalitis. They also mentioned PIMS which I’d never heard of. Heart echo scan done, the doctor examined Maddie again and as she was able to mover her neck normally, he said he was now sure it was PIMS and didn’t need do the lumbar puncture. Things settled down a bit overnight and her temperature started to drop but soon went high again despite having regular paracetamol. The next day we were moved from HDU to another room as Maddie seemed slightly better, However, early hours of the next morning her blood pressure was getting dangerously low and her heart was racing, so she was moved back to HDU and was given 5 large syringes of IV fluids in an attempt to bring her bp back up. She found this very distressing; her bp started to improve but then plummeted again over the next 12 hours.
The doctors were in regular consultation with Birmingham Children’s hospital PIMS team. Maddie wasn’t responding to the current IV antibiotics so she was started on another course of a different antibiotic in the hope it would start working. She’d had the maximum dose of fluids so I was keeping everything crossed her bp would start to stabilise. Thankfully it did as it was looking like Maddie would need to be transferred to the Children’s hospital within hours; this was 11pm. The next day her bp continued to rise and fall but it was improving, as was her temperature. I started to see our little girl’s character again. Thankfully the two different antibiotics worked and Maddie continued to improve and get better. Sunday the 23rd we were allowed to take Maddie home overnight with canula in place as she needed one final dose of IV antibiotics the following day. We returned to the hospital at 11am, then after her last lot of IV antibiotics she was discharged. Maddie has seemingly bounced back very quickly - to look at her know you wouldn’t know how unwell she was just over a week ago. She’s on aspirin and omeprazole for 6 weeks and needs two further heart echo scans. It’s been the scariest most worrying week of my life.
Harry’s Story, age 8, told by his mum, Jenni
My son Harry tested positive for Covid on 23rd September 2021. On 22nd October we took our son to the doctors, following an early morning call to 111 as he had a temp and aching neck. They said it was a viral infection and 2-3 days of rest should be fine.
My son Harry tested positive for Covid on 23rd September 2021. On 22nd October we took our son to the doctors, following an early morning call to 111 as he had a temp and aching neck. They said it was a viral infection and 2-3 days of rest should be fine.
We went off on our half term holiday, thinking a few quiet days would be good for us all. However, by Monday morning he was not better and complaining of additional aches and pains, including some when going to the toilet. We called 111 and we were asked to take him to Chesterfield A&E (nearest hospital). He was admitted later that afternoon with a suspected UTI. However following further assessment and blood tests in the early hours of Tuesday morning they diagnosed him with PIMS-TS. (They had also considered sepsis and Kawasaki, but settled on PIMS.) As he was really poorly we were told he needed to be in a cardiac/specialist hospital they would find space at the nearest hospital as he was not well enough to be sent closer to home.
Our son was transferred on 26th October via the Embrace team (specialized patient transport) to Leeds PICU (Paediatric Intensive Care Unit) for treatment. He remained there until Saturday 30th, when we were transferred to a ward for further monitoring.
He was finally discharged on Monday evening (1st November) and we were able to bring him home on 2nd, as it was a 4 hour car journey. He was discharged with steroids, aspirin and medicine to help his tummy, with instructions to go for blood tests later that week and a heart scan the following week. No other guidance on aftercare. We had to chase to get the appointments confirmed.
Medically, my son is doing well. After a follow up scan in December, he is off all meds. However psychologically it’s a very different case - he is suffering from mental and physical fatigue, mood swings are quite epic some days. They are getting less extreme, but we are working with his school to get him support to manage his frustrations/emotions, as he is struggling to rationalize a lot of things in his head. The consultant from Leeds has been very supportive and unfortunately has more experience with PIMS patients; whereas our local consultant in Swindon has limited knowledge so struggles to know what advice to give.
We have our next scans in March/April, but that's about it from a follow up perspective, so we do feel a bit out on a limb. My son also has mild asthma, so I’ve been speaking to his nurse to make her and the doctor’s surgery aware of what to look for with other possible cases. My main aim would be to raise awareness - early diagnosis is critical and minimizes longer term complications. My son is getting there and making good improvements every day, but is still a long way off being able to do everything he was doing prior to PIMS.







