
Shining a light on PIMS-TS
( Paediatric Multi-inflammatory Syndrome temporally associated with SARS-CoV-2 )
( Paediatric Multi-inflammatory Syndrome temporally associated with SARS-CoV-2 )
Diagnosis
Prompt diagnosis is ABSOLUTELY KEY to ensure prompt treatment and best outcomes for children with PIMS-TS.
- PIMS-TS at its most acute stage can be life threatening and will usually require hospital or PICU treatment to bring it under control.
- The multiple symptoms that both separately and in groups mimic other conditions can easily be misdiagnosed and unnecessary surgery can be undertaken for example appendix removal.
- The longer the inflammatory process goes unchecked, the more potential damage to vessels and organs can occur.
In May 2020, soon after PIMS-TS was identified, the RCPCH (Royal College of Paediatrics and Child Health) published detailed Diagnostic and Treatment protocols for PIMS-TS which we understand were distributed directly to all medical settings. This was followed up with a consensus management pathway for PIMS.
RCPCH-COVID-19-Paediatric-multisystem-inflammatory-syndrome-20200501.pdf
TheLancet-article/PIIS2352-4642(20)30304-7/fulltext
These publications are useful tools, assuming medical staff at all levels have sight of them and have training to apply and embed them.
Unfortunately, through the testimony of families whose children have contracted PIMS-TS, we are seeing a high misdiagnosis rate at all clinical levels. Some staff have not even heard of PIMS-TS. See this parent testimony from 2022.
RCPCH-COVID-19-Paediatric-multisystem-inflammatory-syndrome-20200501.pdf
TheLancet-article/PIIS2352-4642(20)30304-7/fulltext
These publications are useful tools, assuming medical staff at all levels have sight of them and have training to apply and embed them.
Unfortunately, through the testimony of families whose children have contracted PIMS-TS, we are seeing a high misdiagnosis rate at all clinical levels. Some staff have not even heard of PIMS-TS. See this parent testimony from 2022.
In a recent poll in the PIMS-TS family support group showed the following results from 116 responses:
78% didn’t know what PIMS was before their child became ill
51% were misdiagnosed by a GP
24% were misdiagnosed by 111
40% were misdiagnosed by A&E
30% were misdiagnosed by a paediatrician
26% were misdiagnosed twice
14% were misdiagnosed more than three times
This is the experience of some of our PIMS families:
“I called 111 four times during these 5 days and each time they thought he had Gastroenteritis”
“This sadly seems to be the repeated story for many of us. It was 5 days and 4 appointments before my son was admitted to hospital. By that point he was severely unwell, ended up on a ventilator and was in hospital for nearly 3 weeks”
“So many of us were initially turned away or misdiagnosed - after all this time, this shouldn't be happening anymore!”
“I called 111 four times during these 5 days and each time they thought he had Gastroenteritis”
“This sadly seems to be the repeated story for many of us. It was 5 days and 4 appointments before my son was admitted to hospital. By that point he was severely unwell, ended up on a ventilator and was in hospital for nearly 3 weeks”
“So many of us were initially turned away or misdiagnosed - after all this time, this shouldn't be happening anymore!”
This is a very sensitive subject, as families are of course forever grateful to the wonderful NHS staff who helped treat their child in such traumatic circumstances.

We also know that PIMS-TS, like Kawasaki Disease is not easy to diagnose. But we need to do better. Prompt diagnosis and treatment is key to best outcomes for children.
To achieve this, we are calling for -
To achieve this, we are calling for -
- A national public awareness campaign to ensure parents, who are their children’s first responders, know what to look for and have the confidence to ask, “Is it PIMS?”
- Medical staff at all levels need reinforcement of PIMS-TS diagnostic and treatment protocols. These reminders need to be sent direct to them as a matter of urgency.
- Diagnosis/misdiagnosis rates for PIMS-TS cases need to be monitored, and training and support put in place as and when necessary.
- Specialist Hospitals, who are currently supporting smaller regional hospitals on an informal basis, need to be supported to continue and extend this roll.
How a PIMS-TS diagnosis is made
The following diagnostic pathway is informed by the RCPCH diagnostic protocols, with the addition of simple suggestions in red based on the experience of families who have been through PIMS.
Most children present with a high fever, 38.5-40.1 for several days, which is hard to control with over-the-counter medications. Lots of common childhood conditions involve a fever, but a high unrelenting fever for more than 3 days in conjunction with any other the other symptoms should prompt you to seek medical advice. The role of primary care (GPs, pharmacists and 111) and urgent care (paramedics and A&E) is to assess and resolve, or assess and escalate as necessary. The role of secondary care and tertiary care (hospitals and PICUs) is to run tests to further refine the possible cause, then diagnose and treat.
The following diagnostic pathway is informed by the RCPCH diagnostic protocols, with the addition of simple suggestions in red based on the experience of families who have been through PIMS.
Most children present with a high fever, 38.5-40.1 for several days, which is hard to control with over-the-counter medications. Lots of common childhood conditions involve a fever, but a high unrelenting fever for more than 3 days in conjunction with any other the other symptoms should prompt you to seek medical advice. The role of primary care (GPs, pharmacists and 111) and urgent care (paramedics and A&E) is to assess and resolve, or assess and escalate as necessary. The role of secondary care and tertiary care (hospitals and PICUs) is to run tests to further refine the possible cause, then diagnose and treat.
You will instinctively know that your child is unwell with PIMS, so follow your parental instinct. You are a really important part of the PIMS-TS diagnosis process. Keep a record of all symptoms as they happen and take photos if you can. Be informed, ask questions, prepare to be assertive if necessary.
At this point, you will probably find yourselves seeking advice from primary care ie: GP or 111. If this is not in an in- person consultation, it is even more important that you share all the symptoms you have observed and recorded to create a complete picture. These are some of the symptoms seen most commonly at the very beginning of illness as stated by our members: high unremitting fever, lethargy, headache, vomiting, abdominal pain, rash, swollen lymph node in neck, red eyes. These do not necessarily arrive altogether and can appear as the illness progresses. For a more complete range of symptoms see our diagnosis wheel below.
At this point, you will probably find yourselves seeking advice from primary care ie: GP or 111. If this is not in an in- person consultation, it is even more important that you share all the symptoms you have observed and recorded to create a complete picture. These are some of the symptoms seen most commonly at the very beginning of illness as stated by our members: high unremitting fever, lethargy, headache, vomiting, abdominal pain, rash, swollen lymph node in neck, red eyes. These do not necessarily arrive altogether and can appear as the illness progresses. For a more complete range of symptoms see our diagnosis wheel below.
The single most important question that should be considered by parents and medics at this stage is “Could your child have had COVID, or been in close contact with someone who had COVID in the last 6 weeks?” If so, the next question to ask is “Could it be PIMS?”
This won’t rule out other conditions, but it will put the likelihood of PIMS, linked to COVID-19 in a pandemic, higher up the agenda. Essentially, at this stage, it is important to rule out PIMS and other similar acute conditions such as Sepsis and Meningitis to know whether accelerated care is required or not.
In our opinion, if the care is not accelerated at this stage, parents should be given advice on what to look out for PIMS, Kawasaki Disease, Meningitis and Sepsis and advised on what to do should they see these symptoms.
If your care is accelerated to Secondary care or Tertiary care, assessments and tests should then be carried out to further define the cause. Secondary care medics, particularly in paediatric care will probably/hopefully have seen cases of PIMS by now. But if you have read this section of the website, please still ask “Could it be PIMS?” as misdiagnosis is still occurring at all levels. The more informed both parents and medics are and the more they work as a team, the quicker the diagnosis, the quicker the treatment and the better the outcomes.
Your child will probably be more seriously ill by now. It is obviously important to know what you are treating before you treat it, and serious illness calls for serious medications which should not be used out of context as they can be dangerous. Diagnosis needs to be carefully made and sometimes this will take a little while, which can cause anxiety in parents. That is the moment to join our support group.
This won’t rule out other conditions, but it will put the likelihood of PIMS, linked to COVID-19 in a pandemic, higher up the agenda. Essentially, at this stage, it is important to rule out PIMS and other similar acute conditions such as Sepsis and Meningitis to know whether accelerated care is required or not.
In our opinion, if the care is not accelerated at this stage, parents should be given advice on what to look out for PIMS, Kawasaki Disease, Meningitis and Sepsis and advised on what to do should they see these symptoms.
If your care is accelerated to Secondary care or Tertiary care, assessments and tests should then be carried out to further define the cause. Secondary care medics, particularly in paediatric care will probably/hopefully have seen cases of PIMS by now. But if you have read this section of the website, please still ask “Could it be PIMS?” as misdiagnosis is still occurring at all levels. The more informed both parents and medics are and the more they work as a team, the quicker the diagnosis, the quicker the treatment and the better the outcomes.
Your child will probably be more seriously ill by now. It is obviously important to know what you are treating before you treat it, and serious illness calls for serious medications which should not be used out of context as they can be dangerous. Diagnosis needs to be carefully made and sometimes this will take a little while, which can cause anxiety in parents. That is the moment to join our support group.
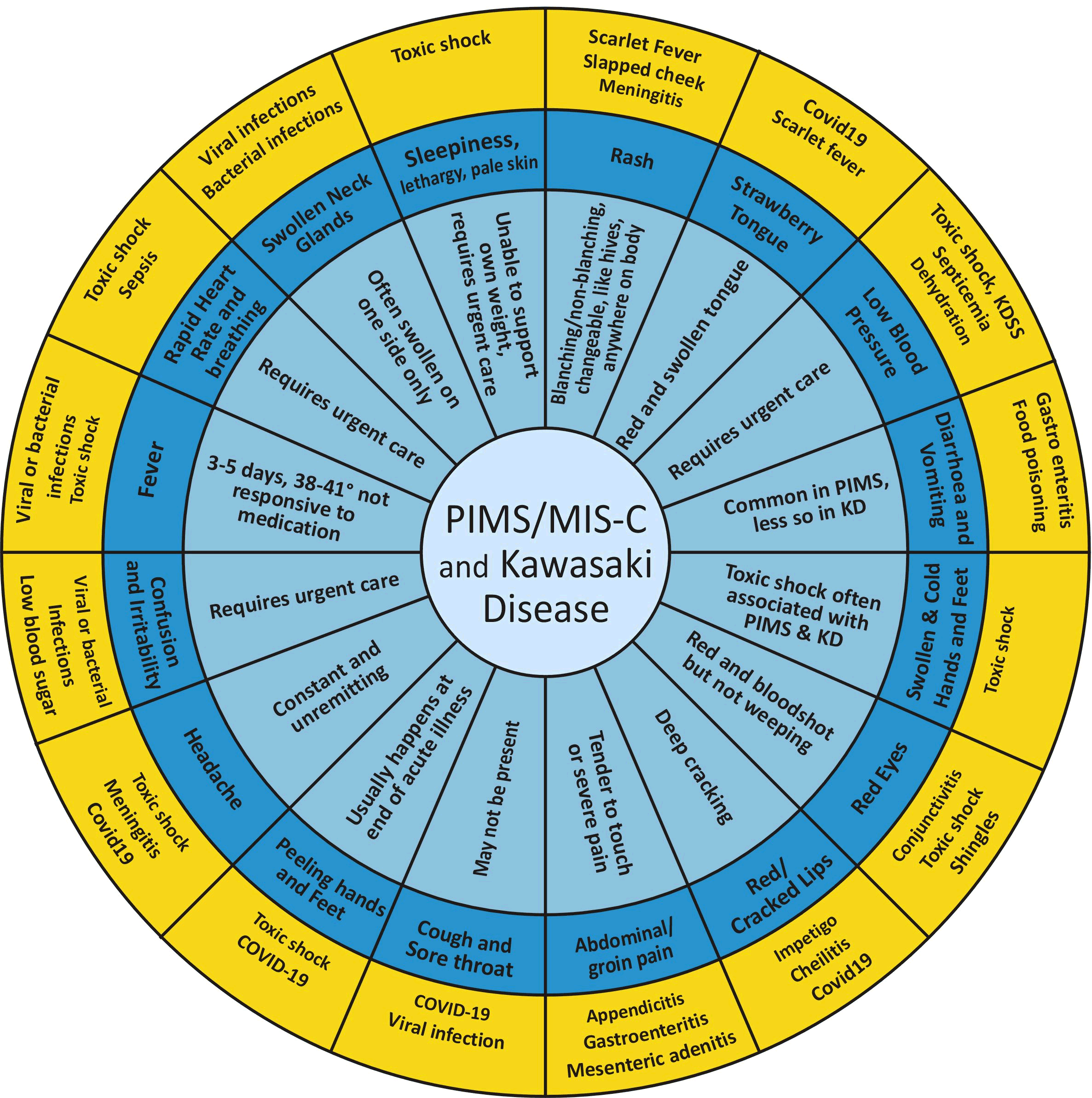
The diagram below illustrates how difficult it is to diagnose conditions such as PIMS with multiple symptoms that overlap with many other conditions, on their own or in conjunction with others.
How to use this wheel
The dark blue circle contains symptoms your child might have. The outer, amber circle, indicates diagnoses other than PIMS. If PIMS (or Kawasaki disease) is suspected, head towards the centre of the wheel.
The dark blue circle contains symptoms your child might have. The outer, amber circle, indicates diagnoses other than PIMS. If PIMS (or Kawasaki disease) is suspected, head towards the centre of the wheel.
If your child is now seriously unwell and you have sought urgent medical help, please also join our Facebook group. We are here to support you, with our lived experience, alongside medical support. We also stay up late!!
If you think your child may have had PIMS-TS in the past and not been diagnosed, follow this link for advice and information.
Clinical tests
The following tests will be taken, some general and some specifically for PIMS-TS as set out in the RCPCH diagnostic tests.
In simple terms:
- Physical examination, rash/glands/tenderness/
eyes/lips/tongue etc - Temperature
- Blood tests to eliminate microbial infection and check for inflammatory markers, falling blood cell counts, rising ferratin, rising D dimers, low sodium, high CRP
- Blood pressure/ heart rate
- Oxygen levels
- Ultrasound scans (ECHO)
- ECGs
- COVID infection and COVID antibody tests
Treatment
Treatment of PIMS-TS follows a similar pattern to the treatment of Kawasaki Disease which is also an inflammatory syndrome.
The treatments which can be used are:
- IVIG (Intravenous Immunoglobulin)
- Corticosteroids
- Aspirin
- Tocilizumab
- Anakinra
- Infliximab
The medical interventions which are sometimes used are:
- Respiratory support
- Invasive ventilation
- Vasoactive support
- CPAP
- ECMO
- Induced coma








